  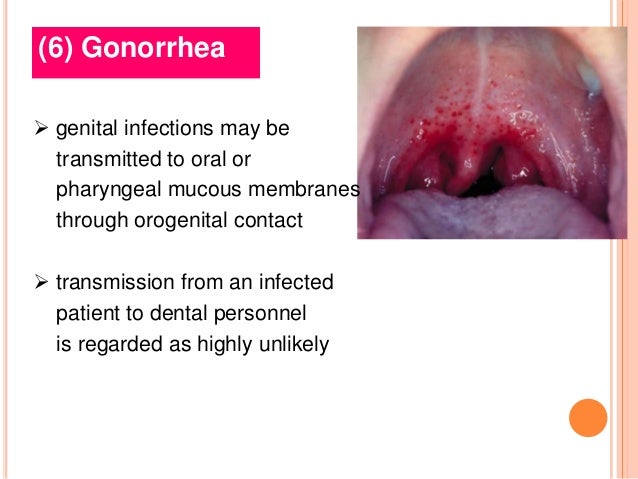
Even when women do have symptoms, they can be mistaken for a bladder infection or other vaginal infection, so that’s testing is important. Yearly gonorrhea testing is recommended for all sexually active women younger than 25 years, as well as older women with risk factors such as new or multiple sex partners, or a sex partner who has a sexually transmitted infection (STI). It may be helpful to speak to your healthcare provider about what testing options they have available. 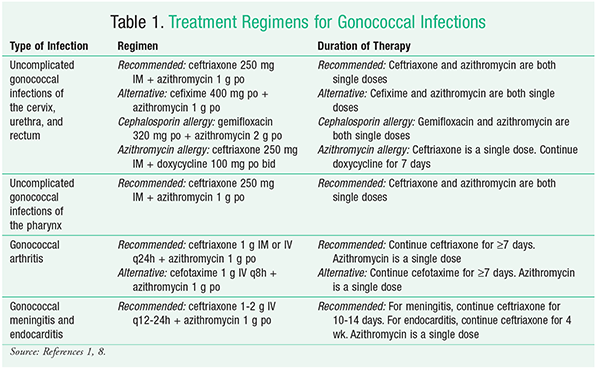
There are different testing options for gonorrhea such as urine or swab tests. Since symptoms may not be present, the only way for a person who has been at risk for gonorrhea to tell whether they’re infected is to be tested. A culture test is used to determine if gonorrhea is causing these symptoms. Gonorrhea infections of the mouth and throat also usually have no symptoms, but a person may experience soreness and redness in the mouth or throat. If there are symptoms, they may include anal or rectal itching, discharge, and pain during defecation (pooping). In about 90% of cases, there are no symptoms. It is possible to have a rectal or anal gonorrhea infection. Others may have one or more of the following symptoms, which can be a sign that the infection has progressed to pelvic inflammatory disease (PID): lower abdominal pain, lower back pain, pain during intercourse, bleeding between menstrual periods, nausea, fever. When the infection spreads to the fallopian tubes, some women still have no signs or symptoms. Abnormal discharge from the vagina that is yellow and sometimes bloody.Women are usually asymptomatic, but might experience: Yellowish-white discharge from the penis.In females, symptoms develop within 10 days of infection. If there are symptoms, they typically show in two days to five days in males, with a possible range of one to 30 days. Many people with gonorrhea are asymptomatic, which means they don’t show any symptoms of infection. Detailed STD facts - HIV/AIDS and STDs.Sometimes, there are no symptoms. doi:10.1007/s40585-4Ĭenters for Disease Control and Prevention (CDC). Pathogenic interplay between Chlamydia trachomatis and Neisseria gonorrhoeae that influences management and control efforts-More questions than answers? Curr Clin Micro Rpt. The presentation, diagnosis, and treatment of sexually transmitted infections. Wagenlehner F, Brockmeyer N, Discher T, Friese K, Wichelhaus T. STDs during pregnancy - CDC detailed fact sheet. doi:10.15585/mmwr.rr7004a1Ĭenters for Disease Control and Prevention (CDC). Sexually transmitted infections treatment guidelines. Gonococcal infections among adolescents and adults. Sexually transmitted infections treatment guidelines, 2021.Ĭenters for Disease Control and Prevention. doi:10.1038/s4157-6Ĭenters for Disease Control and Prevention. Unemo M, Seifert HS, Hook EW, Hawkes S, Ndowa F, Dillon JR. The duration of pharyngeal gonorrhea: a natural history study. StatPearls Publishing 2022.īarbee LA, Soge OO, Khosropour CM, et al. Gonococcal conjunctivitis in adults: Case report and retrospective review of cases in Alberta, Canada, 2000–2016. UpToDate 2023.īelga S, Gratrix J, Smyczek P, et al. Patient education: Gonorrhea (beyond the basics). Oropharyngeal gonorrhea in absence of urogenital gonorrhea in sexual network of male and female participants, Australia, 2018. doi:10.3748/41.15262Ĭornelisse VJ, Bradshaw CS, Chow EPF, Williamson DA, Fairley CK. Sexually transmitted infections of the anus and rectum. StatPearls Publishing 2022.Īssi R, Hashim PW, Reddy VB, Einarsdottir H, Longo WE. Diagnosis and management of gonococcal infections. Gonorrhea - Reported cases and rates of reported cases by state, ranked by rates, United States, 2021. Multi-drug resistant gonorrhea.Ĭenters for Disease Control and Prevention. Centers for Disease Control and Prevention. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
